Hello and a warm welcome to yet another issue of Health Matters, your weekly column that brings you insightful news about health and its related issues.
In our today’s edition, we bring you a presentation by Dr. John Egbuta, Director of ICCIDD delivered at a two-day training for journalist on USI and IDD organized by NaNa and UNICEF.
The presentation provides a global overview of the disorders caused by iodine deficiency.
Special emphasis will be put on recent developments such as the role of iodine deficiency in the development of brain damage and mental retardation, assessment of the iodine status of a population, strategies for control and monitoring of the iodine deficiency disorders (IDD).
Severe iodine deficiency in pregnancy: cretinism and increased fetal and perinatal mortality
The most serious adverse effect of iodine deficiency is damage to the fetus. Iodine treatment of pregnant women in areas of severe deficiency reduces fetal and perinatal mortality and improves motor and cognitive performance of the offspring.
Severe iodine deficiency in utero causes a condition characterized by gross mental retardation along with varying degrees of short stature, deaf mutism, and spasticity that is termed cretinism. These disorders are described in detail below.
Mild-to-moderate deficiency in pregnancy
The potential adverse effects of mild-to-moderate iodine deficiency during pregnancy are unclear. Maternal subclinical hypothyroidism (an increased plasma concentration of thyroid-stimulating hormone in the second trimester) and maternal hypothyroxinemia (a free T4 concentration <10th percentile at 12-week gestation) are associated with impaired mental and psychomotor development of the offspring (31, 32).
However, in these studies, the maternal thyroid abnormalities were unlikely to be due to iodine deficiency. In Europe, several randomized controlled trials of iodine supplementation in mild-to-moderately iodine deficient pregnant women have been done (33).
Iodine reduced maternal and newborn thyroid size, and, in some, decreased maternal TSH. However, none of the trials showed an effect on maternal and newborn total or free thyroid hormone concentrations, the most important outcome (34), and none measured long-term clinical outcomes, such as maternal goiter, thyroid autoimmunity, or child development.
Iodine deficiency in the child
There is cross-sectional evidence that impairment of thyroid function evidenced in mothers and neonates in conditions of mild-to-moderate iodine deficiency affects the intellectual development of their offspring. Aghini-Lombardi et al. (44) reported that in children aged 6-10 years in an area in Tuscany who had mild iodine deficiency (64 ?g iodine/day), the reaction time was delayed compared with matched controls from an iodine sufficient area (142 ?g iodine/day).
The cognitive abilities of the children were not affected. Similarly, it was reported that in an area of Southern Spain with mild iodine deficiency (median urinary iodine of 90 ?g/L), the intelligence quotient (IQ) was significantly higher in children with urinary iodine levels above 100 ?g/L (45)
A recent randomized controlled study in Albania in a moderately iodine deficient area showed that information processing, fine motor skill and visual problem solving improved in school-children after iodine repletion of the population (46). As these anomalies were reversible, they probably result from lately acquired and reversible subclinical hypothyroidism, rather than from fetal and/or neonatal hypothyroidism.
Iodine deficiency in the adult
Anecdotal reports suggest that there is a high degree of apathy in populations living in severely iodine deficient areas. This may even affect domestic animals such as dogs (25). It is apparent that reduced mental function due to cerebral hypothyroidism is widely prevalent in iodine deficient communities with detrimental effects on their initiative and decision-making. Thus, iodine deficiency can be a major block to the human and social development of communities and constitutes a major teratogen at the community level (63).
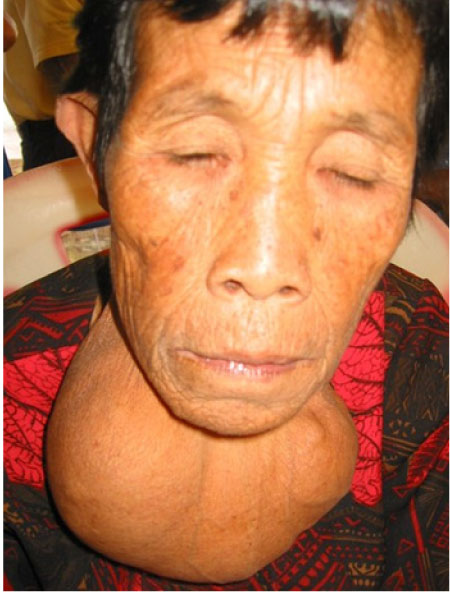
Iodine deficiency at any period in life, including adulthood, can produce goiter with mechanical complications and/or thyroid insufficiency. Another consequence of longstanding iodine deficiency in the adult (64-67) and child (68) is the development of hyperthyroidism, especially in multinodular goiters with autonomous nodules. The pathogenesis of this syndrome is discussed later in this chapter, in the section on side effects of iodine supplementation.
SPECIFIC IODINE DEFICIENCY DISORDERS
Endemic goiter is characterized by enlargement of the thyroid gland in a significantly large fraction of a population group, and is generally considered to be due to insufficient iodine in the daily diet. Endemic goiter exists in a population when 5% of 6-12 year-old children have enlarged thyroid glands.


